Antibiotic resistance is becoming a pressing public health crisis, with an alarming rise in infections caused by bacteria that no longer respond to existing treatments. In 2023, more than 2.8 million antimicrobial infections occurred in the U.S., resulting in over 35,000 deaths, according to antibiotic resistance statistics from the CDC. This surge can be attributed in part to the misuse and over-prescription of antibiotics, including the rising concern of doxycycline resistance among bacteria causing gonorrhea. Research on antibiotic resistance continues to illuminate the complex relationship between bacterial evolution and the efficacy of our medications, highlighting challenges like multidrug-resistant tuberculosis (MDR-TB) that threaten to overwhelm healthcare systems. Without appropriate funding for new antibiotics and innovative research, the very foundation of modern medicine could be at risk, leading to dire consequences for countless patients.
The issue of antibiotic resistance, often described using terms like drug resistance or antimicrobial resistance, is a multifaceted dilemma affecting global health. As pathogens evolve, they increasingly outsmart the antibiotics designed to combat them, leading to a rise in conditions like multidrug-resistant infections. Scientists stress the necessity of new approaches and ongoing funding to address these urgent challenges effectively, especially given the devastating impact of cuts to antibiotic research. Conditions such as extensively drug-resistant tuberculosis pose severe threats, necessitating a robust and well-funded response. Understanding the dynamics of how bacteria develop resistance and implementing comprehensive strategies is critical for safeguarding public health and ensuring effective treatment options for all.
Understanding the Rise of Antibiotic Resistance
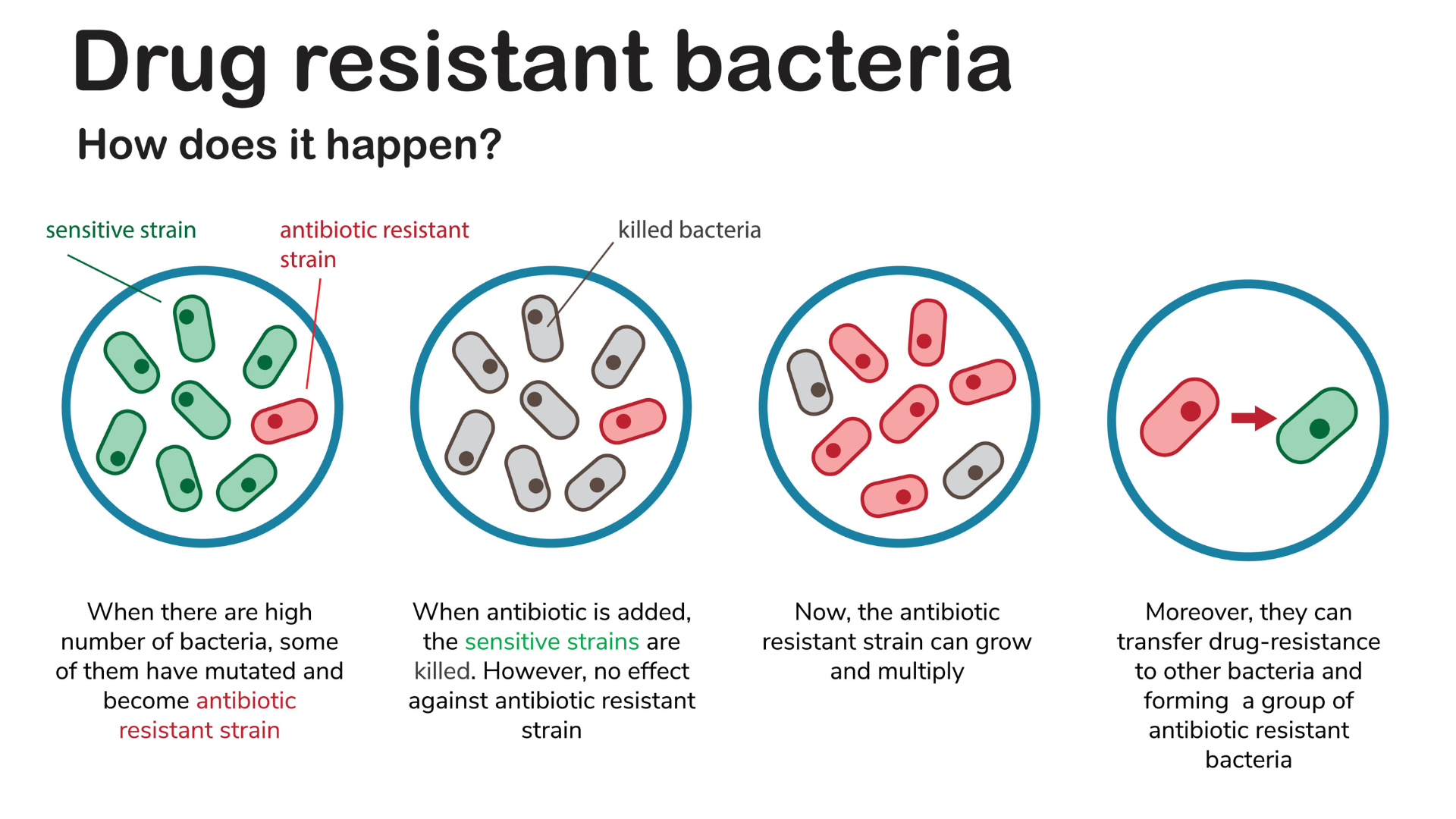
Antibiotic resistance is a growing concern globally, as bacteria evolve to survive the treatment designed to kill them. In recent years, statistics reveal alarming trends; for instance, resistance to doxycycline, commonly used to treat STIs such as gonorrhea, has surged. Research indicates that as of 2024, over 30% of Neisseria gonorrhoeae samples have developed resistance to this antibiotic, raising significant alarm among health professionals. This evolution is not merely a statistic but a reflection of how microbial pathogens adapt rapidly to survive against therapeutic agents that were once reliable.
Furthermore, the consequences of antibiotic resistance extend far beyond infectious diseases. According to CDC data, the United States faces over 2.8 million antimicrobial infections annually, culminating in approximately 35,000 deaths due to resistant strains. This emphasizes the urgent need for enhanced research on antibiotic resistance which can lead to more innovative treatment protocols and strategies. By examining the factors contributing to antibiotic resistance, including the impact of prescription practices and the mutation rates of bacteria, researchers can better formulate solutions to combat this growing epidemic.
The Consequences of Funding Cuts on Antibiotic Development
The ongoing battle against antibiotic resistance is intricately tied to funding for research and development. Experts like Andrew Myers emphasize the critical need for financial support in developing new antibiotics, as many existing drugs are over 50 years old and increasingly ineffective against emerging pathogens. Recent funding cuts from the Trump administration have jeopardized the progress made in antibiotics research, particularly in creating new classes like lincosamides. Without sustaining funding for innovative research, the pathway to developing effective medications could stall, creating a potential health crisis.
Moreover, these funding shortfalls have far-reaching implications, especially in tackling pathogens like Mycobacterium tuberculosis, the agent of tuberculosis (TB). Carole Mitnick’s studies on multidrug-resistant tuberculosis (MDR-TB) highlight how slashes to global health funding can lead directly to increased resistance rates due to incomplete treatment regimens. For instance, with the loss of USAID funding, critical programs that were vital for delivering effective treatments in underprivileged areas face cancellation, thus exacerbating the issue of MDR-TB along with a looming risk of greater antimicrobial resistance.
The Importance of New Antibiotics and Research Strategies
The emergence of antibiotic-resistant infections necessitates the urgent introduction of new antibiotic therapies. Research indicates a critical disparity between current treatment options and the rapid development of bacterial resistance. To counter this, a dual strategy proposed by researchers entails introducing new antibiotics not only as replacements but also in combination with existing drugs. This approach, as outlined in recent studies, could slow down the resistance rates significantly and keep crucial treatment options viable for longer periods.
Recent mathematical models from Yonatan Grad’s team challenge the traditional conservation practices that recommend withholding new antibiotics until older drugs fail completely. Such a change in strategy could drastically alter the landscape of antibiotic usage and retention. Continuing to innovate in the fields of microbiology and pharmacology will be essential to ensure that the healthcare system can effectively respond to an evolving bacterial landscape, making research into antibiotics more vital than ever.
The Global Impact of Multidrug-Resistant Tuberculosis
Multidrug-resistant tuberculosis (MDR-TB) epitomizes the challenges posed by antibiotic resistance on a global scale. With an estimated half a million new MDR-TB cases arising each year, and 150,000 deaths reported in 2023, the imperative for effective global health strategies is undeniable. The situation is exacerbated by the persistent funding cuts and insufficient infrastructure, as evidenced by the stalling of medication deliveries in regions relying on aid. Tackling MDR-TB requires a multifaceted approach, addressing not only drug development but also public health initiatives, patient education, and access to care.
Moreover, the characteristics of MDR-TB illustrate the complexities that researchers face. The diverse bacterial population within infected individuals results in various drug resistance patterns that complicate treatment strategies. Standard regimens are long and can lead to poor patient compliance, thereby increasing the risk of resistance. Collaborative efforts across global health networks are essential for finding and implementing sustainable solutions to prevent the rise of new resistant strains, ensuring that effective treatments remain available.
Community Awareness and the Fight Against Antibiotic Resistance
Community awareness plays a pivotal role in combating antibiotic resistance. Educational campaigns can empower individuals with knowledge about antibiotic stewardship and the risks associated with misuse or overuse of these drugs. Increasing the understanding of how infections spread and the importance of completing prescribed antibiotic courses can significantly curtail unnecessary prescriptions and the subsequent development of resistance. Partnerships between healthcare providers, schools, and community organizations can foster a more informed population that actively participates in combating this public health threat.
In addition, awareness initiatives must highlight the significance of regular screenings and preventative measures for STIs and other bacterial infections. This is particularly vital given the rise in infections such as syphilis and gonorrhea, which saw prevalence rates surge in recent years despite the overall decrease in STIs. By educating the public on these issues, we can create a culture that prioritizes early diagnosis and treatment, reducing the burden of infections and ultimately decreasing the strain on our antibiotic resources.
Innovative Research Approaches to Overcoming Resistance
Innovative research approaches are underway to address the critical challenge of antibiotic resistance. Scientists are employing advanced genomic techniques to explore how bacteria adapt and develop resistance mechanisms. By decoding the genetic makeup of resistant strains, researchers can better understand the evolutionary pathways these microbes take and identify potential targets for new antibiotic classes. This research not only promotes a deeper understanding of resistance but also lays the groundwork for crafting precise and effective treatment regimens that can outpace bacterial evolution.
Moreover, interdisciplinary collaborations are proving essential in the fight against antibiotic resistance. By merging insights from microbiology, pharmacology, and even data science, researchers can devise novel strategies to combat resistant bacteria. For instance, the development of synthetic biology techniques allows scientists to engineer bacteria that can produce new antibiotics or enhance the efficacy of existing drugs. With such collaborative efforts, the potential for discovering groundbreaking therapies increases, providing hope for managing infections that currently lack viable treatment options.
Future Directions in Antibiotic Research
Looking ahead, the field of antibiotic research must pivot towards sustainability and adaptability in response to the escalating threat of resistance. Future strategies will likely emphasize the need for rapid drug development cycles, ensuring that newly created antibiotics remain effective for as long as possible. This necessitates a shift in both research funding priorities and public health policies to support ongoing innovation and the rapid integration of new findings into clinical practice.
Additionally, cultivating a robust pipeline of new antibiotics means investing not just in immediate solutions but also in foundational research that enhances our comprehension of bacterial biology and resistance mechanisms. Engaging younger scientists and fostering an environment of innovation are crucial for sustaining a workforce committed to tackling antibiotic resistance. As resistance evolves, so too must our strategies, ensuring that future generations will have the tools they need to manage infections effectively.
Policy Recommendations for Addressing Antibiotic Resistance
Formulating effective policy recommendations is imperative in the overarching strategy to combat antibiotic resistance. Proactive policies should focus on increasing funding for antibiotic research, ensuring that scientific endeavors are supported adequately to explore innovative solutions and secure health against resistant pathogens. This includes advocating for public-private partnerships aimed at fostering collaboration between researchers and pharmaceutical companies to expedite the development of new antibiotics.
Moreover, implementing global initiatives such as the One Health approach can integrate efforts across human, animal, and environmental health sectors, recognizing the interrelated factors contributing to the emergence of antibiotic resistance. Policymakers have a vital role in encouraging responsible antibiotic usage in agriculture, food production, and clinical settings. By uniting these efforts globally, we can create a comprehensive framework to reduce the threat posed by antibiotic-resistant infections and safeguard public health.
Frequently Asked Questions
What are the current antibiotic resistance statistics in the U.S.?
In 2023, there were over 2.8 million antimicrobial infections in the U.S., resulting in more than 35,000 deaths, highlighting the urgent problem of antibiotic resistance.
What does recent research on antibiotic resistance reveal about the effectiveness of doxycycline?
Recent studies indicate that resistance to doxycycline, especially in gonorrhea infections, is increasing rapidly, emphasizing the need for continuous monitoring and new treatment strategies to combat antibiotic resistance.
How does multidrug-resistant tuberculosis impact global health?
Multidrug-resistant tuberculosis (MDR-TB) affects approximately 500,000 new cases each year and led to an estimated 150,000 deaths in 2023, showcasing its significant challenge in the fight against antibiotic resistance globally.
What is the impact of funding cuts on antibiotics and antibiotic resistance research?
Funding cuts for antibiotic research have been significant, threatening the development of new antibiotics and advancements in fighting antibiotic resistance, as highlighted by the termination of crucial NIH grants.
How can the rapid development of antibiotic resistance affect treatments for infections?
The quick evolution of antibiotic resistance means that once effective treatments may soon become ineffective, leading to higher morbidity and mortality rates from bacterial infections if new antibiotics aren’t developed.
| Key Point | Details |
|---|---|
| Current STI Statistics | In 2023, 2.4 million cases of syphilis, gonorrhea, and chlamydia were diagnosed in the U.S., but this marked a 1.8% decrease from 2022. |
| Antibiotic Resistance Mechanism | Bacteria develop resistance to antibiotics, including doxycycline, which is crucial for treating STIs. |
| Historical Context | Antibiotics have revolutionized medicine since the introduction of penicillin; however, every antibiotic eventually leads to bacterial resistance. |
| Antibiotic Prescription Increase | Doctors wrote 252 million antibiotic prescriptions in 2023, increasing from 613 to 756 per 1,000 people. |
| Ongoing Battle Against Resistance | Researchers like Yonatan Grad track resistance development and strategize the introduction of new drugs to outpace bacteria. |
| Consequences of Funding Cuts | Cuts to research funding threaten the development of new antibiotics and can have dire public health implications. |
| Public Health Concerns | Approximately 500,000 new cases of multidrug-resistant tuberculosis (MDR-TB) occur yearly, with high mortality rates. |
| Community Engagement | Activism, exemplified by the TBFighters, is working to reduce testing costs for diseases like tuberculosis. |
Summary
Antibiotic resistance is a critical global health issue, driven by the rapid evolution of bacteria against our available treatments. As antibiotic prescriptions rise, so does the challenge of managing resistant strains that can render common infections untreatable. The continuous battle against antibiotic resistance necessitates sustained investment in research and development to ensure effective therapies remain available for future generations. Without timely and adequate funding for antibiotic development, the medical community faces the risk of regressing to a time when infections could lead to severe morbidity and mortality.