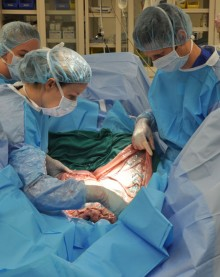
CALEC surgery, or cultivated autologous limbal epithelial cell surgery, is revolutionizing blindness treatment by providing hope to patients with severe corneal damage. This innovative procedure, developed at Mass Eye and Ear, utilizes stem cell therapy to repair the corneal surface safely and effectively. By extracting healthy limbal epithelial cells from a patient’s unaffected eye and cultivating them into a graft, CALEC surgery offers a potential path to restore vision when traditional methods fall short. Clinical trials have demonstrated exceptional results, with more than 90% success rates in repairing corneal injuries, marking a significant breakthrough in ocular regenerative medicine. As research progresses, CALEC surgery stands at the forefront of cornea restoration, potentially transforming the lives of those afflicted by debilitating eye conditions.
The groundbreaking technique known as CALEC surgery is also referred to as cultivated limbal stem cell therapy, an advanced method in the field of ocular regenerative treatments. Utilizing limbal epithelial cells harvested from the patient’s healthy eye, this innovative approach provides a novel solution for treating severe corneal damage that often leads to blindness. The process involves creating a cellular graft that can be surgically implanted into the damaged cornea, facilitating its restoration. With a remarkable success rate in clinical trials, this treatment represents a new era in blindness intervention strategies, highlighting the potential of stem cell therapies in rejuvenating vision and enhancing quality of life for patients suffering from debilitating eye diseases.
Overview of CALEC Surgery
Cultivated autologous limbal epithelial cells, known as CALEC surgery, represents a groundbreaking advancement in the field of ocular regenerative medicine. This innovative procedure involves harvesting healthy stem cells from a patient’s unaffected eye, which are then expanded in a laboratory setting to create a cellular tissue graft. The hallmark of CALEC lies in its ability to restore the damaged cornea in patients suffering from limbal stem cell deficiency, a condition that previously left many individuals with permanent visual impairment. With a significant success rate exceeding 90%, CALEC is emerging as a beacon of hope for those who have long struggled with corneal injuries.
The safety and effectiveness of CALEC surgery have been substantiated through a series of clinical trials, the first of which was led by researchers at Mass Eye and Ear. The clinical study followed 14 participants over 18 months, documenting significant improvements in corneal surface restoration and visual acuity. Ula Jurkunas, the principal investigator, highlighted the clinical trial’s success, stating that nearly 50% of participants experienced a complete restoration of their cornea within just three months, evolving into higher success rates as time progressed. This innovative approach not only addresses the urgent need for new blindness treatment options but also showcases the potential of stem cell therapy as a vital tool in ocular medicine.
The Role of Stem Cell Therapy in Ocular Medicine
Stem cell therapy stands at the forefront of modern medicine, particularly in the realm of ocular therapies. In the context of cornea restoration, stem cells play a crucial role in regenerating limbal epithelial cells, which are integral to maintaining the cornea’s smooth surface. As highlighted in the groundbreaking CALEC surgery, stem cells harvested from a healthy eye can be manipulated to create grafts that restore function to a damaged eye. With the increasing understanding of stem cell applications, researchers are exploring how these therapies can treat various ocular conditions, which historically limited patients’ vision and quality of life.
Furthermore, as researchers delve deeper into ocular regenerative medicine, the focus remains on expanding the effectiveness of stem cell therapies. Collaborative efforts among institutions, such as the partnerships between Mass Eye and Ear, Dana-Farber Cancer Institute, and Boston Children’s Hospital, highlight a comprehensive approach to solving complex eye disorders. The findings from CALEC surgery trials emphasize this need, showcasing how stem cell therapy can evolve to address a wider range of blindness treatment options, potentially leading to allogeneic processes that could utilize donor tissue to benefit even more patients suffering from corneal damage.
Challenges and Future Directions for CALEC Surgery and Stem Cell Therapies in Ophthalmology
While CALEC surgery has shown remarkable success in preliminary trials, there are ongoing challenges that must be addressed to make this treatment widely available. Currently, the procedure requires that patients have only one eye affected by damage, as a biopsy from the healthy eye is necessary to harvest the limbal stem cells. This limitation poses difficulties for many patients suffering from bilateral cornea damage, underlining the pressing need for further research. Future studies aim to develop allogeneic methods wherein stem cells are collected from deceased donors, thereby expanding the eligibility criteria and enabling more people to benefit from this potentially life-changing therapy.
Additionally, researchers are keen on increasing the scale of clinical trials for CALEC, allowing for a broader patient demographic and more extensive data collection over extended periods. As Ula Jurkunas has expressed, the goal is to lead CALEC towards FDA approval, legitimizing this treatment as a standard practice in ophthalmology. With continuous advancements in stem cell technology and deeper insights into ocular regenerative medicine, the future looks promising for those seeking relief from previously untreatable corneal injuries.
Understanding Limbal Epithelial Cells and Their Importance
Limbal epithelial cells are a critical component of the eye, primarily located at the junction between the cornea and the sclera. These cells are responsible for maintaining a healthy corneal surface and play a significant part in healing eye injuries. When individuals experience damage due to trauma, chemical burns, or infections, the depletion of these vital cells can lead to limbal stem cell deficiency. This condition creates a challenging barrier for potential treatments, often leaving patients with chronic pain and impaired vision that conventional interventions cannot remedy.
In the context of CALEC surgery, understanding the role of limbal epithelial cells becomes paramount. By utilizing stem cell therapy to regenerate these cells, researchers have taken a significant step toward restoring not just vision but the quality of life for those affected. As the approach to limbal stem cell therapy evolves, the advances in creating and transplanting CALEC grafts underscore the critical need for continued research in this area. Enabling regeneration of these cells through innovative techniques holds the potential to revolutionize blindness treatment and ocular medicine as a whole.
Research Collaborations and Future Prospects
The development of CALEC surgery is a testament to the power of collaborative research in advancing medical science. The pioneering work conducted at Mass Eye and Ear involved significant partnerships with institutions like Dana-Farber Cancer Institute and Boston Children’s Hospital. Such collaboration enriches the research process by bringing together diverse areas of expertise, which is essential for exploring innovative solutions in ocular regenerative medicine. This multi-disciplinary approach has not only propelled the CALEC trial but has set a standard for future research endeavors aimed at enhancing treatment methodologies for corneal damage.
Further exploration into the capabilities of stem cell therapies is underway, driven by positive feedback from initial clinical trials. This research collaboration model not only fuels scientific discovery but also aims to address the larger systemic issues within healthcare concerning access to such advanced therapies. As more data becomes available, and with the ambition to expand CALEC protocols to accommodate a wider range of patients, the goal is to transform this innovative procedure into a broadly accessible treatment option that can significantly improve life for those facing vision loss.
Frequently Asked Questions
What is CALEC surgery and how does it relate to stem cell therapy?
CALEC surgery, or cultivated autologous limbal epithelial cells surgery, is an innovative procedure that uses stem cell therapy to treat cornea injuries considered untreatable. It involves harvesting limbal epithelial cells from a healthy eye to create a graft that can restore the surface of a damaged cornea, significantly improving vision and quality of life for patients suffering from blindness due to corneal damage.
How effective is CALEC surgery in treating corneal damage?
CALEC surgery has shown remarkable effectiveness in clinical trials, with over 90 percent success in restoring the cornea’s surface. In studies, complete restoration was noted in 50 percent of participants at three months, increasing to 79 percent at 12 months and 77 percent at 18 months, making it a promising option in ocular regenerative medicine.
Who is a suitable candidate for CALEC surgery?
Ideal candidates for CALEC surgery are those with limbal stem cell deficiency caused by corneal injuries such as chemical burns or trauma. It is essential for candidates to have at least one healthy eye from which limbal epithelial cells can be harvested. This surgical procedure offers hope for patients with corneal damage that could not be treated by traditional methods.
What is involved in the CALEC surgery process?
The CALEC surgery process includes a biopsy to collect limbal epithelial cells from the healthy eye, which are then cultured to expand into a cellular graft. After 2 to 3 weeks, this graft is surgically transplanted into the damaged eye. This innovative approach leverages stem cell therapy to effectively restore the cornea’s surface.
Are there any risks associated with CALEC surgery?
While CALEC surgery has a high safety profile with no serious adverse events reported, like all medical procedures, there are risks involved. The most common risks include minor complications or infections, such as a bacterial infection linked to chronic contact lens use. Patients are carefully monitored to manage any potential adverse effects.
When will CALEC surgery be widely available?
Currently, CALEC surgery is classified as experimental and is not available in hospitals across the U.S. Further studies with a larger patient population are required for potential FDA approval. Researchers aim to enable wider access to this effective treatment option in the future.
What impact does CALEC surgery have on vision improvement?
Patients undergoing CALEC surgery have shown varying levels of improvement in visual acuity following transplantation. The clinical trial results indicate that the treatment not only restores the corneal surface but also significantly enhances the visual capacity of individuals suffering from corneal damage.
How does CALEC relate to blindness treatment options?
CALEC is a significant advancement in blindness treatment, specifically for those suffering from cornea damage due to limbal stem cell deficiency. By utilizing innovative stem cell therapy, CALEC offers a new pathway for restoring vision in patients who previously had limited options for effective treatment.
| Key Point | Description |
|---|---|
| First CALEC surgery performed | Conducted by Ula Jurkunas at Mass Eye and Ear. |
| Innovative stem cell therapy | Uses cultivated autologous limbal epithelial cells (CALEC) to treat corneal injuries. |
| Clinical trial success rate | Over 90% effectiveness in restoring corneal surfaces after 18 months. |
| Patient eligibility | Requires patients to have only one uninjured eye for harvesting stem cells. |
| Future implications | Plans to develop allogeneic manufacturing process for broader patient treatment. |
| Regulatory status | Currently experimental; not yet available at U.S. hospitals. Further studies needed. |
Summary
CALEC surgery represents a significant breakthrough in the field of ophthalmology, specifically for treating severe corneal injuries that were once deemed untreatable. This innovative procedure utilizes stem cells from a healthy eye, offering hope to patients and emphasizing the potential of regenerative medicine. As research continues and further trials are conducted, CALEC surgery may soon pave the way for greater accessibility and effectiveness in treating corneal damage, enhancing the quality of life for those affected.